Preparing for Relapses
Like any health problem, in schizophrenia relapses often tend to strike when you are least expecting them. When a health crisis occurs it often makes day-to-day living really difficult especially if you find that you are not able to get out of the house or if your emergency relapse plan requires you to stay at home for a while. Of course when we are well we don’t like to think about things going wrong but that is precisely the best time to make a few sensible preparations for when we are not able to function so well. Remember the maxim: we hope for the best but prepare for the worst. Below are a few ideas to help you get ready for the time when a mental health problem or physical illness prevents you from living your normal life.
Relapse Planning
It is really vital to work out in advance what steps you will take if the signs of a relapse begin to appear. Remember you may not be able to function well when it does happen and at that time may not be able to work out what to do. By knowing in advance what to do you will reduce the risk of dangerousness and minimise the damage that the relapse will do to your life. When you start to put this plan together you should discuss it with your community psychiatric nurse or social worker if you have one along with your carers and relatives.
There are four parts to a successful relapse plan:
1. Spotting the signs early.
2. Getting professional help quickly.
3. Seeking sanctuary.
4. Self help.
The first part is spotting the danger signs. For this you will first need to know what the danger signs are and this will vary from person to person. For instance you may begin to notice that you are getting paranoid thoughts again or that you have started to hear voices. It is a good idea to use a method of continuously monitoring your residual symptoms such as the methods in our information sheet on self monitoring. Whatever method you use the key point is to have worked out well in advance what signs indicate that you are becoming unwell so that you can activate your relapse plan quickly.
The next part of the plan is getting professional help quickly. Schizophrenia is such a massive threat to our health that we cannot be expected to battle it successfully on our own and we need to organise all the help we can to get through a relapse. We should not feel guilty about asking for help. Access to health care is, in this society, our right and mental health problems are no different to physical ones in this respect.
If you are still in the mental health system then your community psychiatric nurse, psychiatrist or social worker will be the first port of call. If you have been discharged from the mental health system then you should contact your GP, mental health gateway (if your area has one) or out-of-hours social worker. However, if you feel that you are really moving fast into a serious crisis then go to A&E at the local hospital and ask to see the duty psychiatrist.
Remember, do not delay getting help. If you think that you are confronting an imminent relapse then it is best to get help quickly and not take a wait-and-see approach.
Next there is the need to seek sanctuary. By and large it is best, if a relapse is impending, not to stay on at work or be out and about around the town but to try to go to somewhere safe and peaceful where you can relax and avoid things that may provoke psychotic thinking. Usually this will be your own home but alternatively it could be the home of some other person close to you such as a parent if they agree.
Lastly there is self help. Above all at this time self help is key to successfully managing your relapse. The first thing to do is to speak to your doctor or CPN about adjusting the dose of your medications temporarily until the symptoms are once again under control. Next think about talking therapies to help with the symptoms. This could be arranging to see a good counsellor or your existing one if you have one or going to a support group. This is also the time to make use of your support network by telling your friends and family that you are becoming unwell. By taking an active role in managing your relapse you will be helping the professionals to help you and taking ownership of your recovery.
Advance statements and directives
An advanced directive or advanced decision is a document that you make when you are well in which you can opt to refuse certain kinds of treatment in the future when you become ill. An advance directive is legally binding and cannot be overridden by doctors unless you have been sectioned.
An advance statement on the other hand is a document that you write while you are well that gives the doctors and health care workers advice about what you would like to happen if you become unwell. It is not legally binding on the doctors but nowadays doctors are coming to realise that they are a useful part of the overall therapeutic strategy and are treating them with more respect.
Part of the statement is simply about routine issues such as whether you have any pets and who you would like to look after them if you go into hospital. However the statement can also contain significant and useful information that the doctors can use to make your treatment as effective and beneficial as possible. This could be advice about how your illness has developed over time, what sort of symptoms you suffer from and what treatments have worked well for you in the past.
An advance statement does not need to be drawn up by a solicitor, you can do it yourself. The Colebrook organisation in the West of England has produced a useful booklet to help with drawing up an advance statement.
Power of attorney
A power of attorney (P.o.A.) is a legal document which enables another person to make decisions on your behalf when you become so ill that you are not able to make good decisions yourself. There are two types of power of attorney: one dealing with health and welfare and the other dealing with finances and property.
A power of attorney is a very powerful document that you should give a lot of thought to if you think that you need one. However if you have had a problem of getting into debt during previous periods of ill health you may find that it is an extremely useful way of preventing this happening again. Similarly if you had problems of being evicted from your home or had your home threatened with re-possession when you have been poorly before you may find it a very useful precaution to take.
This type of document allows you to appoint someone else (called the attorney) to run your finances or make decisions about other aspects of your life when you become ill. The other person could be a relative or close friend but clearly they must be someone who you know extremely well and trust absolutely.
When making a power of attorney you can specify exactly what you want the attorney to do. For instance you could give them the ability to look after your bank account and pay your bills using the money in your account. The power of attorney has the weight of law behind it and any decisions that the attorney makes on your behalf must be respected by for instance your bank or utility companies.
There are two ways of making a power of attorney. An individual can make a power of attorney using the forms available on the .Gov website. There is a fee for registering the P.o.A. Alternatively, a solicitor can be used to draw it up and they will charge for this work. Some solicitors will carry out this work on a pro bono basis, that is at a reduced fee or no fee at all, or you may be able to find a law centre that will carry the work out at no cost. In deciding which method to use it is important to realise that a P.o.A. is a very powerful document and if you are not entirely confident it is best to take appropriate professional advice. In any case, before making a P.o.A. it is vital to give it a great deal of thought and to find out as much about the process as possible. Organisations like Citizens Advice would be a good place to start. Although P.o.A.s can be very useful they do have potential pitfalls and they must only be made with very careful thought and preparation and where necessary with appropriate professional advice from a qualified person.
More about powers of attorney is available on the .gov website and the Citizen’s Advice website.
Getting Help
Making a ‘phone call in an emergency
You may need to get in touch with someone close to you or with your doctor or nurse in an emergency and find that your mobile has run out of charge or you are in an environment such as a hospital where use of mobiles is not allowed. For this reason it is a good idea to keep a paper list of your important telephone numbers on a slip of paper in your wallet or purse. This list should include your next of kin, some close friends, GP, CPN (community psychiatric nurse) and social worker. You may also like to include the number for the local out-of-hours social worker, NHS Direct and the Samaritans along with a number for the local branch of any mental health charities such as Mind that may be able to help. You should also keep some small change to enable you to make a call from a public telephone.
It will also help if you keep a paper copy of your prescription in your wallet or purse as well. If you are admitted to hospital in an emergency you will be asked for details of any medications you are currently taking and if you are on several types it may be difficult to remember them all so having a paper copy of the script will help the medical staff to get you help more quickly.
Put ICE into your mobile
ICE stands for: “In case of Emergency”. Many people nowadays put the number of someone close to them who they would like to be called if they were taken poorly into their mobile under ICE instead of the person’s name. Police and ambulance paramedics dealing with unconscious casualties are now trained to check the person’s mobile for an ICE number.
The Medicalert Scheme

Medicalert medallions are a simple way of making sure that you get help quickly in an emergency. They are also available as bracelets. (Image: Medicalert)
Medicalert is an international database of people with health conditions. It is not run by the government or the health service but by an independent charity set up in 1953. When you join the scheme you tell them your personal details such as name, address and date of birth along with details of your health condition, medication and someone who you would like to be told if you are taken ill. You will then be given a card to carry in your wallet or purse which will contain your scheme registration number and an international telephone number. Health care workers in any part of the world can call this number 24 hours a day to find out about your health conditions and get you help more quickly particularly if you are unconscious at the time you are admitted. The Medicalert operators can speak in over 100 languages so this help is available across the world.
You can also buy a medallion which you can wear around your wrist or on a chain around your neck which is engraved with your scheme number and the Medicalert telephone number. These medallions are one of the first things that ambulance paramedics and staff in A&E are trained to look for if they have an unconscious patient.
Membership of Medicalert costs around £30 per year but for people on some benefits free membership is available under a sponsorship scheme run by the Lions Club.
Here’s what one person living with schizophrenia said about his Medicalert membership:
“I wear my Medicalert medal everywhere. It gives me the re-assurance of knowing that if I ever fall ill or get injured they can get me the help I need sooner rather than later”.2
Useful resources
Support network
While you are well and healthy is a good time to start to build a circle of people around you who can look out for you and help you when you are unwell. This support network may contain members of family, existing friends or new friends that you have made while you have been in the mental health system. With existing friends it may be necessary for you to tell them about your diagnosis so that they can help you better when the time comes. If you decide to do this it should be done very carefully. Our information sheet on disclosure contains some more information on this aspect.
You should spend some time while you are well thinking about how each of these people could help you during a relapse event, after all you do not want to impose on them. Some people may find it quite easy to cope with the seeing psychotic symptoms in others whereas some may find it difficult to cope with. On the other hand some of your friends may have useful resources such as a car and could possibly help with lifts to appointments or running small errands for you if you can’t get out of the house. Others, particularly close friends or family, may be able to provide an all important shoulder to cry on when things get really unbearable. Your support network is one of the most important resources you have and building a really good one is an important part of recovery.
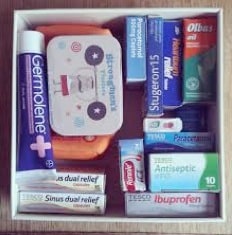
A simple home medicines kit with over–the-counter remedies for everyday ailments.
Medication
Some people find that It is a good idea to keep an emergency stock of medication in their home in case they are taken ill and can’t get out of the house. About 14 days worth is about right. This should include prescription medicines along with any over-the-counter remedies. Before doing this you must speak to your GP or CPN and always follow their advice. Most will be very happy to help by providing an additional prescription for this purpose and will be very pleased that you are taking an active role in managing your condition.
In general you should aim to keep a well-stocked medicine cabinet with a few simple remedies for everyday minor ailments such as colds and stomach bugs. Remember to keep an eye on the expiry dates and rotate your medicines by using the oldest first.
Food
A small stock of emergency food kept in the home in case you are not able to get out to the shops for a while is a very good idea. If you have a freezer or frozen food compartment in your fridge you could keep some fresh food such as a pint of milk and half a loaf of bread. However you can also keep a stock of dried and tinned foods. Aim to keep enough food in your emergency store for three days as this will give you a breathing space to make alternative arrangements for your shopping such as shopping on line and having it delivered.
Here are some useful foods to keep in your emergency stock:

Keep a small stock of tinned and dried food in case you aren’t able to get out to the shops. (Image: MAHATHIR MOHD YASIN/Shutterstock)
Baked beans
Tinned meat such as Spam or corned beef
Tinned potatoes and vegetables
Biscuits and crackers
Tinned fruit
Tinned custard
UHT milk or tinned milk
Tinned soups
Breakfast cereal
Utilities
If you are taken ill and have to stay at home for a while you may have difficulty paying for electricity and gas particularly if you pay using a card or key meter. Spending a day or night without any electricity or in the cold is liable to seriously exacerbate any health problem you may have so it is important to always keep an emergency amount of credit on your key or card. Again 14 days worth is about right.
Cash
If you can’t get out of the house to do your shopping for a while you may have friends or neighbours who would be willing to run a few small errands for you. You will then have to reimburse them and it is not a good idea to get into debt. So keep a small reserve of cash in the house to cover this. It should not be so much that it creates a security risk but it should be enough to allow for about a week of being confined to the house. It is best not to tell anyone about this money and to keep it somewhere secure, if possible locked away.
References
1. This information sheet is based on the author’s personal experiences.
2. Conversation with person with schizophrenia. February 2014.







